To what extent has the UK seen cuts in spending to the NHS and health care spending in recent years?
In short:
- Actual spending on the NHS has increased.
- Real spending per capita has been broadly flat in recent years.
- As a share of the nations wealth, it is falling and it is true to say there have been cuts to health care spending as a % of GDP.
- In addition “non-NHS” spending e.g. public health services and capital spending have seen cuts to budgets in certain years.
- A problem for NHS is that demand is growing faster than supply due to a rise in incidence of diseases such as obesity, diabetes, cancer and auto-immune diseases. This means that increases in health care spending might not meet the rising demand and we get longer waiting lists (and pre-waiting lists) – despite higher spending.
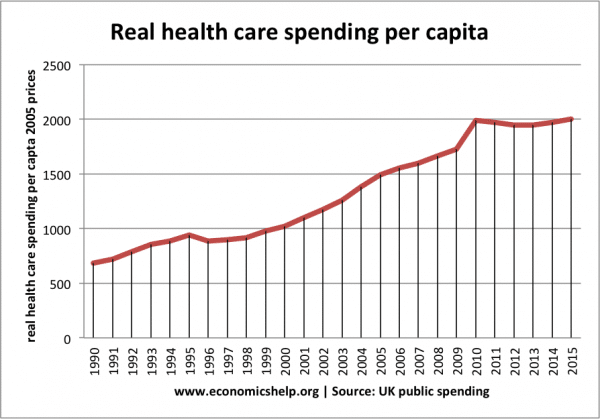
Real spending on the NHS
Real spending takes into account the effects of inflation and is best measure for spending in constant prices.
Real spending on the NHS has increased consistently and shows NHS spending has risen faster than the average price level.
2010-2015, real spending on the UK NHS grew by 0.84 per cent per year (Kings Fund) But, this is the lowest growth in spending since the Second World War.
For the next parliament, the government have stated real NHS spending will rise £10 billion by 2020/21. (Kings Fund) £8bn within NHS England.
This would be a growth rate of 1.75 per cent per year. Higher than past parliament, but lower than the post-war average
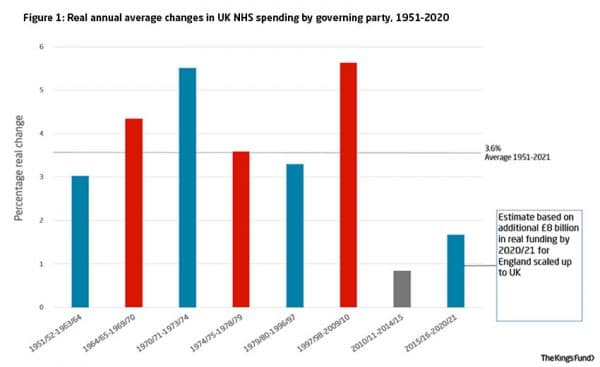
Real health care spending per capita
This is real health care spending divided by the population; the average spend per person.
Between 1990 and 2015, the UK population has risen from 57 million to 64 million so it is important to take into account this rise in the population.
This is an important metric, often ignored. But, if real spending rises 3% and the population rises 3%, then the average spend per person remains unchanged. It also breaks the recent trend for upward real spending per capita.
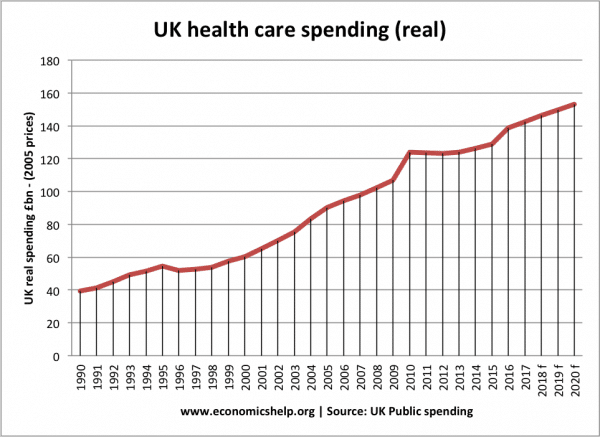
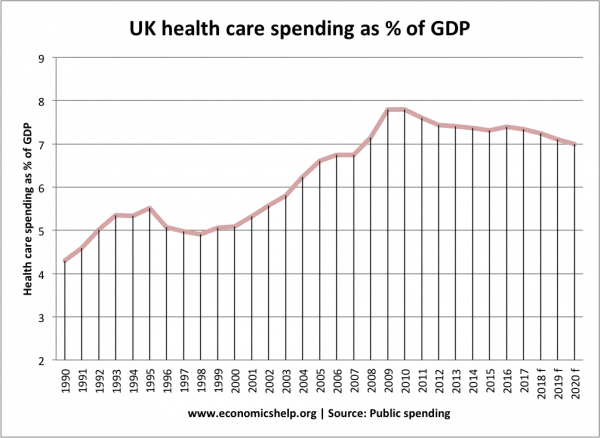
NHS spending as a % of GDP
Another way of measuring the amount of resources devoted to public health care spending is the percentage of health spending as a proportion of GDP (national income).
This shows that between 1990 and 2008, the percentage of resources devoted to public health care spending rose from 4% of GDP to 7% of GDP.
The sharp rise between 2008 and 2010 is a more reflection of the fall in real GDP from recession, than rise in health care spending.
However, the important trend is the decline in health care spending as % of GDP from 2010 onwards. It means a smaller share of the nations wealth is being devoted to health care spending. This reflects the projected governments plans public to reduce public spending as % of GDP.
Spending rising but falling share?
To simplify, the economy is growing by around 2%, but real spending on health is rising by 1%. It means spending is increasing, but the rise in spending is slower than the growth in GDP.
Public health spending
Another issue is that it depends how you classify health care spending. Spending on the NHS could be considered core services, however, there are other aspects of health care spending not included in this core statistic. In 2015, the chancellor announced a cut of £200m from ‘non-NHS’ services (Guardian). This is the public health services concerned with more preventative approaches. For example, campaigns to reduce smoking, tackle obesity, prevent diabetes and prevent unwanted STDs. You could argue this preventative approach could give a more cost-effective approach to the nations health – preventing disease rather than dealing with consequences.
Capital budget
Another area of health care spending is capital spending. This is spending on improving the infrastructure of hospital buildings and machines. It is not included in core “NHS service” but is important for the long-term health of the NHS.
In March 2016 budget, the NHS was expected to be allocated £4.8bn to cover this area, but the health service will only be receiving £3.7bn of capital budget. NHS capital fund at Independent.
Another issue is reclassifying who is responsible for pensions of health care workers. This article suggests the government has placed a greater burden on health employers to be responsible for pensions than the government. (Independent)
Demand for services
- The other issue for the NHS is that demand is not necessarily growing at a constant per capita rate. There are various factor which place greater strain on demand for NHS services. In particular:
- Ageing population. With the UK experiencing an ageing population, it means there will be a relatively greater increase in demand. People over 65 have much greater need of health care services.
- Changes in technology. With improved drugs and technology, doctors have more potential treatments for patients than ever before. But, these cutting edge treatments are often more expensive. Therefore, NHS costs can rise faster than typical inflation because of the increased possibilities.
Conclusion
Real spending on the NHS has increased and will continue to rise. However, it is debatable whether this is enough to meet the needs of a rising population, and rising number of potential treatments.
The UK has a choice, whether to increase the percentage of the nations income on the NHS. There is an opportunity cost – higher NHS spending will require either higher taxes or spending cuts from elsewhere. But, there is also an opportunity cost from squeezing NHS spending – especially public health services – with less scope for preventing diseases, which may increase the burden in the long-term.
On the positive side, the government have protected health care relative to large spending cuts in other departments. There have also been some improvements in public health – through reduced smoking rates and in future the ‘sugar tax’ could play a role in preventing obesity and tooth decay.
But, it is correct to talk about cuts to health care as a % of GDP. The question is what would British voters prefer – this cut to the relative size of the NHS or higher taxes and more spending on health care?
Related

My Comment as economic students , government should find solution to prevent for certain disease like HIV ,Sugar ,stress and lounger rather than spending .
IT would be interesting to compare with other countries, especially America but also within Europe. I understand NHS is the cheapest / most underfunded (delete as appropriate).
having used the N H S a lot lately (I am 86)i think although the service and treatment is first class there is a lot of wastage as in most large organisations. There is also a lot of time wasted on unnecessary paper work. which takes up much of the nursing staffs time.Most of this will never be required .Like pages of blood presures which are out of date etc The data is also put onto computers and never consulted again.The control of materials is poor .Just try and return used equipment like walking sticks etc They are just dumped.